Prosthetic hand research is a hot topic these days. By improving our understanding of the connection between the hands and the brain, we can overcome many of the limitations that have always impeded advancement in prosthetics. And we may well be on our way to developing bionic hands straight out of science fiction.
Fabrice Bares is not a Jedi like Luke Skywalker. But, like the Star Wars character, the 44-year-old Frenchman had his right hand amputated. “My Darth Vader – the science-fiction character who cut off Luke Skywalker’s hand with a lightsaber – was a lawnmower that I had the misfortune of coming too close to when I was 4 years old,” he said on a French television programme in 2014. His case was widely covered by the media, as he was the first patient in France to receive an improved prosthesis, featuring technology that enables him to perform complex everyday tasks, such as tying his shoes or typing on a computer keyboard. After getting by without a prosthesis for nearly 35 years, he “treated” himself to his bionic hand just before his 40th birthday. Looking at himself in the mirror after slipping on his prosthesis for the first time, he finally felt normal, with two legs and two arms. However, there was a disconnect between what his brain perceived and reality. “It’s very disturbing. It’s like having a concrete block around my arm. I feel as though the prosthesis is three times bigger than it really is,” he said on television at the time.
How telling. This type of prosthesis does not allow patients to control their grip or feel the shape and texture of objects. Another problem persists, says Andrea Serino, a neuroscience researcher at the University of Lausanne (UNIL) and Lausanne University Hospital (CHUV). “The vast majority of people who receive prosthetics end up abandoning them.” Researchers and engineers are working to understand why that happens and develop technological solutions to change that.
An opportunity has come for amputees. Neuroscientists view the development of prosthetics as essential for fundamental research. Prosthetics of the future, or so-called bionic prosthetics, guide our questions, such as “How does our brain develop the sense that something belongs to the body?”. Daniel Huber, a researcher from the Department of Neuroscience at the University of Geneva, sees this as a way of studying the genesis of decision-making or how movement is learnt.
Of the many international projects under way, Lausanne has been a pioneer in the area since 2014, through the laboratory led by Silvestro Micera at the Swiss Federal Institute of Technology in Lausanne (EPFL) and its close collaboration with Andrea Serino. In Vivo invites you to explore the futuristic world of prosthetics and bionic hands.

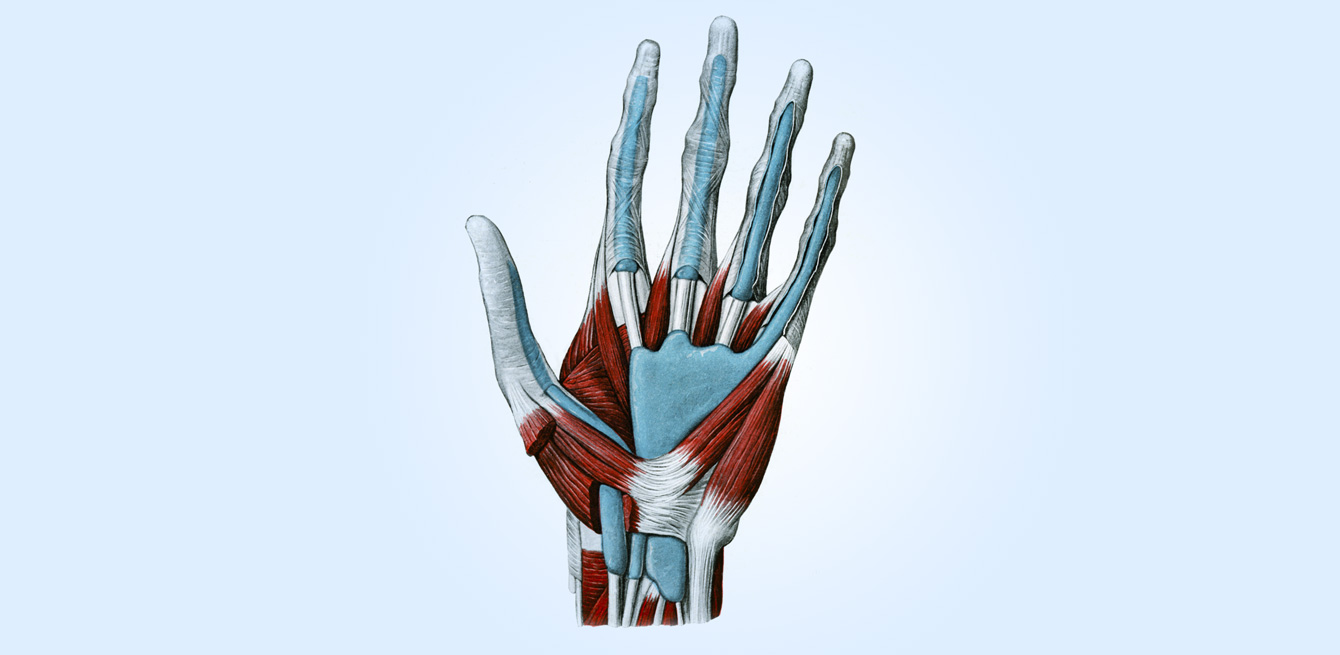
The hand is a very complex structure. “It’s a part of the body with remarkable anatomy, dexterity, sensitivity and developed strength for its size,” says Thierry Christen, a physician with the Service of Plastic and Hand Surgery at the CHUV. To grasp all that subtlety, we need to take a trip to the Department of Fundamental Neurosciences at the University of Lausanne. There, we find the anatomy and morphology room where Julien Puyal, hand anatomy teacher, explains, “It’s the cohabitation of muscles, tendons and joints combined into a strict functional organisation that sets the hand in motion throughout the full extent of its multiple axes of freedom.”
The anatomical complexity of the hand is also reflected in the fact that no less than 36 muscles and 27 articulated bones are coordinated for the hand to perform a simple gripping action and grasp an object.
Even so, reproducing the mechanical complexity of the hand has not seemed to scare away engineers. “It’s not the limiting factor in any case,” says the neuroengineer Silvestro Micera, whose work is supported by the National Centre of Competence in Research (NCCR) Robotics and the Bertarelli Foundation. However, experts are far from being able to imitate the underlying nervous system used to operate this precision machinery with any accuracy.
Muscles are controlled by motor neurons that transmit signals from the brain and spinal cord. The nerves in the hand also contain sensory fibres that send information to the brain. Like electric cables, each individual nerve fibre has a specific motor or sensory role. Some nerves measure several millimetres in diameter, while the fibres they contain are much smaller. Motor neuron fibres are about 20 micrometres in diameter, five times smaller than a human hair, and can transmit signals at a speed of up to 120 metres per second. Depending on the information they send, sensory fibres vary in diameter.
“For example, fibres that send information on pain are among the smallest and can be half a micrometre in diameter – 200 times smaller than a human hair – and perform their task at a speed of 2 metres per second,” Julien Puyal says.
The technical challenge for the prosthetic consists in connecting itself correctly to the size of motor and sensory fibres.
Sensory nerve fibres run directly from the hand to the spinal cord. All the sensory information is then transmitted to the somatosensory cortex in the brain. This part of the cortex devoted to the hand is very large, as its size is proportionate to the number of nerve endings. “The inner side of the fingers can contain up to 2,500 sensory receptors per square centimetre. Comparatively, the same surface on the thigh has about 50 to 100 times fewer receptors,” Julien Puyal says.
The hand motor area in the motor cortex controls motor neurons in contracting hand muscles, where each movement begins. It is important that these decision-making processes in the brain are not unidirectional. “Actually, they function in a loop inside the cortex. The brain uses sensory information to refine movement, the same way it uses movement to predict sensations,” says Daniel Huber, a researcher at the University of Geneva.
To create a bionic hand that resembles the hand of a man or a Jedi, we must be able to transmit sensory information to the cortex so that it can make that hand as realistic as possible.


The several types of prosthetics available on the market are not all designed to achieve the same purpose. Choosing the right prosthesis depends on the patient and individual sneeds. “Not all amputees want the same thing. Some are comfortable and get by with their residual limb; others want a purely cosmetic prosthesis, while still others want to regain functionality,” says Thierry Christen.
Cosmetic solutions have only one purpose: to hide the disability. These prosthetics are modelled after the remaining hand and sculpted in wax. Meanwhile, several myoelectric systems are available to restore some functions of a natural hand. These prosthetics are implanted with two sensors and two electrodes placed on the flexor and extensor muscles in the residual limb. The muscles receive signals to rotate the hand, or open and close it like a clamp.
Several improved prostheses have been available since 2012, like the one used by Fabrice Bares. The prosthetic limbs made by the German firm Ottobock, the world leader on the prosthetics market, can perform 14 movements and reproduce 90% of the gestures of a human hand. But John Spillar, a marketing expert at Ottobock, explains that “when we’re trying to recreate a human hand, the challenge is controlling the different functions, more than the technical capabilities of the prosthetics themselves.”
To improve control, Ottobock developed a pattern recognition system that launched on the market in early 2019. Eight electrodes used to operate the prosthesis measure muscle movement patterns in the residual forearm and are assigned to hand movements.
“When the patient stretches the hand towards a bottle of water, the prosthesis control system recognises the associated movement pattern and automatically gives the order to perform the relevant grip,” John Spillar says.
These sophisticated prosthetics come at a price, valued at several tens of thousands of Swiss francs. But low-cost alternatives, priced at a few hundred Swiss francs, have been designed using 3D printing. These versions can be manufactured fast but can only be used to open and close the hand. They are ideal especially for children, who have to change their prosthesis frequently as they grow. These prosthetics are also easy to put on and take off, and do not require surgery or rehabilitation.
In Switzerland, the Swiss National Accident Insurance Fund covers patient care. A complex process then defines which type of prosthesis will be provided. “Switzerland has relatively few upper limb amputees, certainly because good work safety conditions apply and the country is not at war,” says Sébastien Durand, a surgeon with the CHUV Service of Plastic and Hand Surgery.

As Andrea Serino pointed out, most amputees abandon their prosthesis. “The reason is that they never manage to adopt it or sometimes prefer to get by with their residual limb,” he adds. Many amputees also suffer from phantom limb pain, and the prosthetics, however sophisticated they may be, do not take that pain away.
“90% of amputees feel phantom sensations, and 70% suffer from phantom pain, as if the amputated limb was still there,” Andrea Serino says.
These well-known sensations occur due to the persistent representation of the amputated limb in the brain.
The research carried out by Andrea Serino and his team, in particular Dr Michel Akselrod, aims to understand how the human brain creates the sense of ownership and what neural pathways are engaged. His work has demonstrated that bodily self-consciousness does not only come from the sense of sight but from the integration of multisensory signals. For example, just before the brain sends a motor command to the hand, it predicts the hand’s position. Then a flurry of sensory feedback comes back after the movement is performed. “If the feedback is consistent with the prediction, the brain understands the movement to be its own. If the hand moves to the left, while the brain intended to move it to the right, the sense of ownership of the hand does not occur,” he says.
The sense of touch and sight are therefore fundamental to self-consciousness. This concept was demonstrated with the rubber hand illusion. This well-known test involves individuals who place both hands on a table in front of them. One of their hands is hidden by a panel. A rubber hand is then placed within view, positioned where the hidden hand would be. The researcher then simultaneously stroked a finger on the rubber hand and on the hidden hand with a paintbrush.
“That simultaneous stimulation causes the brain to believe that the rubber hand belongs to it in just a few seconds,” Andrea Serino says.
To demonstrate that, without warning the subject, the researcher suddenly crushes the artificial hand with a hammer. Individuals automatically withdraw their real hand.
“Amputees can’t tolerate their prosthetics because they don’t feel that the prosthesis is part of their body,” the researcher says. With his colleague from EPFL, Silvestro Micera, he has proved that this disconnect comes from sensory information that has been ignored.


The research teams headed by Silvestro Micera are attempting to restore the bidirectional connections between the nervous system and the hand. They are pioneering the development of methods to deliver sensory feedback to a prosthetic user. “Our approach involves embedding the prosthesis with sensors to collect information about the task the hand is performing. We then translate that information into electrical parameters used to stimulate peripheral sensory nerves,” the researcher explains. To do that, stimulation electrodes are placed directly on the nerves, like a small hair with multiple electrical contacts. “As we stimulate each of them one after the other, we simply ask the patients if they feel something, and what the sensation is. We then connect the corresponding prosthetic sensor to the patient’s nervous system.”
Since 2013, four volunteer amputees have received experimental prosthetics developed by Silvestro Micera.
They were used for six months, the duration of the experiment. The sensory feedback helped improve movement quality because patients can adjust the movement based on the feedback. The four volunteers were in turn more efficient. The sense of ownership of the prosthesis, as predicted by Andrea Serino, was much better due to the sensory feedback, and in fact, patients no longer felt any phantom limb pain. The experiment led to a series of scientific publications, namely in the journals Science Roboticsand Neuron, and will be followed up. Researchers are now preparing to implant permanent prosthetics by the end of 2020.
A limited number of sensors was used in these trials, but a real hand can detect vibrations, static and dynamic movement, sensations of touch, pressure and temperature. So, will Luke Skywalker’s bionic hand hit the market one day? Not for another 20 years, experts say. Plus, the sensory complexity of the hand cannot be fully reproduced, as the electrical stimulation is not precise enough to target the small size of a particular sensory fibre. “But we’re already trying to replace our sensors with an ‘e-skin’ and its artificial sensory system developed by researchers in Singapore. Meanwhile, we’re working on increasing the accuracy of stimulation by genetically modifying the sensory fibres in neurons to use light, instead of electricity,” Silvestro Micera says. It is now up to developers of sensors to create more sophisticated systems.
Many research projects currently focus on integrating sensory feedback into hand and other prosthetics.
Ottobock, the market leader, is developing implantable electrodes with “several research institutions to come up with sensory feedback solutions in the medium term,” John Spillar explains. European consortiums such as DeTop and LifeHand2 led by Silvestro Micera have the same strategy. But the projects connect the prosthesis to the nervous system in different ways. Andrea Serino feels that “their main challenge is to determine the minimum combination of sensory inputs and motor commands required to trick the brain into believing that the sensory feedback is real and feeling that the prosthesis is part of the body.”
Number of people worldwide who have had upper limbs amputated.
Percentage of people who wear a prosthesis and suffer from phantom limb pain.
Number of people who have received a bionic prosthesis developed by Silvestro Micera at EPFL.

A severed hand looking for its body was the story line of the animated French film I Lost My Body (J’ai perdu mon corps). After winning this year’s Cannes Film Festival, the film will be running for an Academy Award in 2020.

Number of people who use French Sign Language. Contrary to popular belief, there is no universal sign language but rather families of sign languages and regional variants.
Niccolò Paganini, the great 19th-century violinist, owes part of his musical ability to the shape of his hands. He had hyperextensible joints, allowing him to bend his fingers in exceptional ways.
Three million people worldwide have had an upper limb amputated. According to a report from Pennsylvania State University published in 2015, almost 2.4 million of them live in developing countries. In these countries, more than 75% of partial arm amputations were caused by trauma. Traumatic limb loss mainly occurs in the work environment or war zones, while other causes include congenital diseases, cancer and infectious or cardiovascular diseases. Diseases like these are the main reasons for amputation in developed countries, with the leading cause being cardiovascular complications due to diabetes. The university study states that these types of amputations are not expected to slow with the growth in diabetes due to changing food habits. There are approximately 10,000 new upper limb amputees every year in the United States alone, according to the National Center for Health Statistics.

Re-establishing the connections between the brain and the limbs also helps paraplegic patients. In the STIMO (Stimulation Movement Overground) study published last year, CHUV and EPFL researchers implanted electrodes in the spinal cord of three patients. The devices activate specific areas and reproduce signals that the brain would send to trigger walking. Using this targeted electrical stimulation combined with body weight support therapy, patients were able to walk with crutches or a walker and control the muscles of their legs, which had until then been paralysed.