Advances in research on the genetic and environmental factors that cause schizophrenia could help experts develop new drugs to treat the disease.
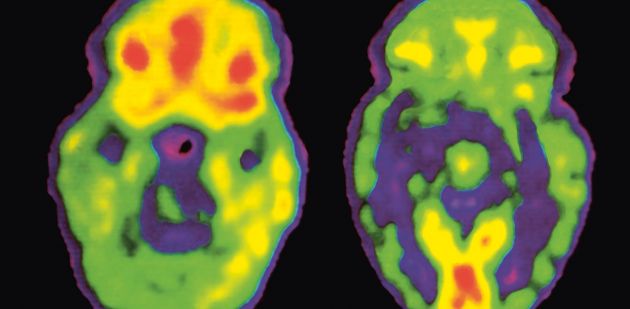
Picture: brain activity in a healthy brain (left) versus a schizophrenic brain (right)
For nearly 15 years in Lausanne, psychiatrists have been working with neuroscientists to better understand schizophrenia. This relatively unique collaboration has resulted in some promising advances. “It may seem logical for neuroscientists and psy-chiatrists to work together,” says Kim Do Cuénod, professor at the Center for Psychiatric Neurosciences at Lausanne University Hospital (CHUV).
“But it rarely happens. By teaming up to study the disease, we can easily compare neuroscientific findings against patient problems.” As a result, she has been able to show the relationship between schizophrenia symptoms
and oxidative stress.
One of the factors that causes schizophrenia could in some cases be genetic. It prevents control of the oxidative balance in the brain, which brings on a whole slew of problems, such as the deterioration of the insulating myelin sheath surrounding nerve cells.
“The nervous system, which accounts for 2% of our body weight but uses 25% of our oxygen consumption, is particularly vulnerable to oxidative stress,” says Kim Do Cuénod. “We’ve observed deficiencies in the antioxidant system in the brain of schizophrenic patients through either brain imaging or cerebrospinal fluid analysis.” This work is conducted as part of the close partnership between the Centre for Biomedical Imaging at the Swiss Federal Institute of Technology in Lausanne (EPFL), in which researchers use imaging to measure antioxidant levels in animal and human brains and in intracerebral connections.
One of the factors that causes schizophrenia could in some cases be genetic. It prevents control of the oxidative balance in the brain, which brings on a whole slew of problems, such as the deterioration of the insulating myelin sheath surrounding nerve cells. This deficit in turn impairs conduction in nerve fibres and disrupts the synchronisation of impulses between the different parts of the brain.
“This discovery could be included in a biomarker profile used to confirm a diagnosis of schizophrenia, which is currently established solely based on clinical symptoms,” Do Cuénod says. But perhaps more importantly, these advances could lead to the development of new treatments. The Lausanne-based researcher and her team have been studying a group of 60 patients receiving care at the Service of General Psychiatry since 2008. A group of them have taken a drug to counter the effects of oxidative stress, and the results are impressive. “We’ve observed an improvement in cognitive abilities and hallucinatory symptoms in patients defined based on markers of blood redox,” the expert says. Neuroleptics, the only drugs currently given to schizophrenics, fail to treat cognitive impairment appropriately. And the medication has a number of side effects, especially on metabolism.
“This discovery could be included in a biomarker profile used to confirm a diagnosis of schizophrenia, which is currently established solely based on clinical symptoms,” Do Cuénod says.
These treatments also offer new solutions for preventing the disease. “We now know that the causes of schizophrenia lie in a complex set of environmental, psychological and genetic factors,” says Philippe Conus, chief of the Service of General Psychiatry at CHUV. “If we could detect high-risk subjects, we could offer them a preventive treatment that would improve the oxidative balance in the brain.” These discoveries have given Philippe Conus a great deal of hope. “Psychiatry has made enormous progress in caring for schizophrenic patients and improving their quality of life. We used to have 700 beds for them here at the Hospital of Cery. Today there are only 95. People either live at home or in a specialised centre.”
But the expert feels that these results, achieved through
a combination of neuroleptics and psychotherapy, are not enough. “Of the patients who experience a first psychotic episode, 30% will recover, 30% will have an intermediate outcome and 30% will experience many subsequent relapses.” Identifying biomarkers and developing early intervention strategies could improve this outlook. ⁄
Schizophrenia is a psychological disease in which a person loses contact with reality. This mental disorder affects about 0.7% of the population, with the first symptoms generally emerging in early adulthood. Schizophrenics typically experience delusions, hallucinations, disorganised thinking and altered emotional expression. Despite common misconceptions, schizophrenia should not be confused with multiple personality disorder or aggressive behaviour.
Cells need a balance between free radicals and antioxidants to function properly. That is what is referred to as redox balance. A redox imbalance can lead to oxidative stress. If this state persists over a long duration or occurs during critical periods in brain development (gestation or the early years of life), it can damage cell membranes, proteins and DNA.
Most experts now agree that schizophrenia is the result of a multitude of genetic, environmental and psychological factors. For example, the vulnerability gene DISC-1 was found to have mutated in a large Scottish family with several members who had been diagnosed with schizo-phrenia. Flu infections, nutritional deficiencies and severe psychological stress during pregnancy have been associated with a higher risk of the disease. Psychological or sexual abuse during childhood and the use of cannabis by children under the age of 14 also increase the likelihood of developing schizophrenia.