Made-to-measure printing techniques are already revolutionising the production of prosthetic limbs and implants. Used with biological materials, this technology could be paving the way for artificial organ generation.
Jul 16, 2014
3D printing is now being used to help research to fight cancer.
Teams of researchers from China and the United States have created models of cancerous tumours using the technique. Until now, only two-dimensional cell culture models have been used. This breakthrough will provide a more realistic image and therefore results. These tumours built in vitro are designed to study the growth and spread of the cancer and the development of new treatments.
Nov 29, 2013
Update: 3D printing is now a reality in the CHUV. The first production (for our maxillofacial surgery service) is on its way. We will present some pictures soon.
Myles Bartlett will never forget his daughter Stella’s reaction the first time she attached her WREX plastic exoskeleton to her arms. “After the initial momentary shock, she picked up a paintbrush and sat painting for over an hour”, says the Canadian. His three-year old girl has spinal muscular atrophy, a genetic condition that affects the way her brain communicates with her muscles. “She is very weak, gets tired quickly and finds it hard to lift her arms”. The WREX allows her to move the upper half of her body, eliminating the effects of gravity. “Now she can eat on her own, raise her hand in class and play with her pals”, he explains. “The WREX has changed her life”.
Yet Stella would never have been able to benefit from this device without the help of a new technology which is revolutionising medicine: 3D printing. “The first version of the WREX, which we produced in 2005, was made of metal”, says Tariq Rahman, the mechanical engineer who developed the invention at Alfred I. duPont Hospital for Children in Wilmington, Delaware, USA. “A child this young would never have had the strength to lift it”.
The engineer then made a WREX from plastic, a more lightweight material, using a 3D printer, a device which produces objects by building up successive layers of liquid plastic. “With this method we were able to customise the exoskeleton so it fits the size of the patient perfectly”, he continues. “We take her measurements and enter them into the computer, which generates a digital 3D model of the WREX and then manufactures it to order using the printer”.
As Stella gets bigger, her mechanical arms can be continually adapted to fit. “The new parts can be sent to us by post and we simply have to screw them to the WREX using a screwdriver”, says Myles Bartlett, smiling. “A few weeks ago a small piece of the exoskeleton broke. I told the hospital on Monday, and received the new part on Wednesday. Without the 3D printer,
it would have taken weeks”.
“It may not be long before 3d printing brings about even more spectacular revolutions in medicine.”
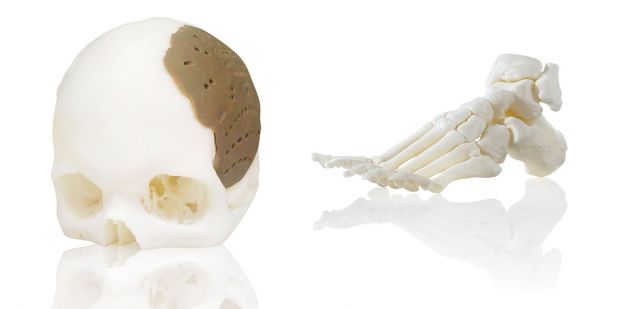
The dental, hearing aid and orthopaedic prosthetic industries were the first to grasp the potential of this new technique. Customised crowns, orthodontic appliances, audio prostheses and artificial limbs have been produced for several years now, using a 3D scan of the patient’s anatomy. More recently, it has been used to improve implants. “We can now produce synthetic, made-to-measure hip implants and spinal discs all in one piece, using the patient’s data”, explains Tim Caffrey, engineer and consultant specialising in 3D printing. “They are a better fit, more solid and less expensive”.
A patient in America has just had 75% of his skull replaced with an implant made of PEKK, a polymer, manufactured using a 3D printer from Oxford Performance Materials (OPM). “This material is much lighter than the metal parts normally used, which can make patients dizzy or give them headaches”, adds Mr Caffrey. In 2012, a team of Dutch doctors implanted a titanium jawbone in an 83 year old woman. The fine mesh structure, which imitates real bone and makes the implant several grams lighter, was possible thanks to 3D printing technology.
This technique has also made it easier to miniaturise certain processes. Kaiba Gionfriddo, just two years old, owes it his life. Born with a malformation of the trachea, he was unable to breathe unaided. “We used an image of his respiratory tract to produce a minuscule splint using a 3D printer, which was implanted into his trachea to keep it open”, explains Scott Hollister, the doctor at the University of Michigan who performed the operation in 2012. “It is made from a polymer which will be reabsorbed by his body in about two years’ time. By then his trachea will have had time to develop properly”.
With 3D bioprinting, cells are built up layer after layer to create living tissue.
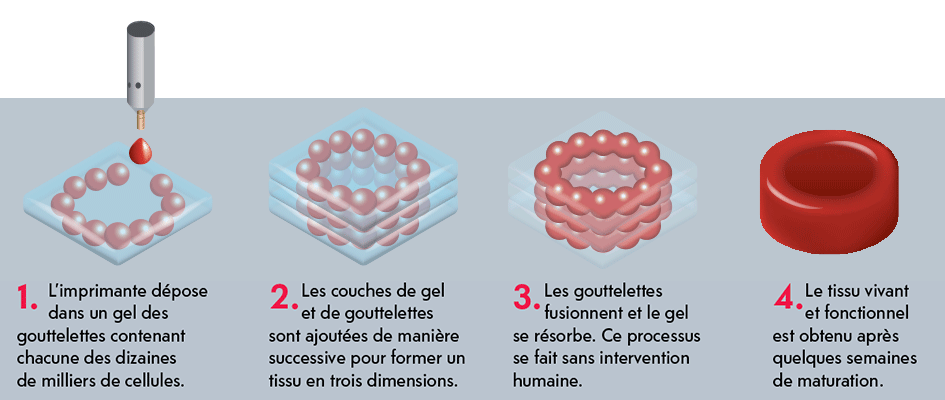
Infography: Sebastian Gagin et Ale Román
At the MetroHealth centres in Ohio, 3D printing is used to improve patient safety. The Reconstructive Maxillofacial Surgery Unit uses it to produce a synthetic model of the face of patients requiring surgery. This allows the surgeons to practice before the actual procedure, determine the least invasive option and even predict in advance what types of bone implants will be needed. “The patient therefore spends less time under anaesthetic and in theatre”, points out Mr Caffrey. The method was used for the first time in 2002, in preparation for a delicate procedure for separating Guatemalan twins who were joined at the skull. The surgery lasted 22 hours “instead of the 97 hours normally required for this type of procedure”, according to Eitan Priluck, founder of Biomedical Modeling, the Boston company which provided the models of the two girls’ skulls.
It may not be long before 3D printing brings about even more spectacular revolutions in medicine. Californian company Organovo, created in 2008, was inspired by research conducted at the University of Missouri and has invented a printer that works using “ink” made of biological materials such as cells. “In particular we have been able to produce fragments of liver tissue, heart muscle and arteries”, explains Eric David, one of the founders of Organovo. “Our clients are research laboratories and pharmaceutical companies wishing to test the efficacy or toxicity of new drugs. These models offer an exact replica of the architecture of human tissue as it is found in the body, unlike the 2D cell cultures normally used”.
Ultimately, Organovo hopes to be able to print a whole
organ, such as a liver or a kidney, and implant it into a
patient. “This would be incredibly valuable, given the lack
of donors”, believes Mr David. Each organ would be made
from the cells of the patient who is going to receive it. “This would avoid the risk of rejection”, he explains. In April, the company announced it had successfully produced a fragment of liver. The tissue had a microvascular network and was able to replicate a large number of the organ’s functions, such as cholesterol production.
Jeremy Mao, a researcher at Columbia University, is in turn interested in the possibilities of printing teeth and bones. “We make a structure from bone or synthetic enamel in the shape of the tissue we want to regenerate, and seed it with the patient’s stem cells”, explains the reconstructive medicine specialist. “It then serves as a mould for differentiating and reconstructing the missing bone or tooth”. So far, the method has only been tested in rats and rabbits, but the initial results are promising. “As the population ages, broken bones and joint replacements will become increasingly common”, notes Mr Mao. “If the body is able to repair these tissues using its own stem cells, it would make the process faster and safer for the patient”.
The possibilities opened up by this research have caught
the imagination. Some believe that we could achieve immortality by replacing organs as and when they wear out. Others dream of overcoming the effects of old age by grafting on a print-out of your face as a teenager. Yet others still are discussing the possibility of saving a copy of all one’s organs and limbs on a computer, so they can be reproduced in the event of an accident or disease.
However, Lee Ann Laurent-Applegate, head of Regenerative Therapy at the Plastic and Reconstructive Surgery department at the Lausanne University Hospital (CHUV), points out that 3D printing using live tissue is still only an experimental technique and has not yet been put to the test. “If the cells have no blood supply, they cannot survive longer than 15 hours”, she warns. “That is how long it takes to produce a 9x12 cm fragment of skin using a 3D printer”. Using this method to treat major burns would be an indulgence, “You would have to wait 4-5 weeks to print enough skin just for one leg”.
“Although 3D tissue printing is not a magical cure, it does pose very interesting possibilities in certain cases, for example if you wish to repair a small area of bone, cartilage or skin or if one day it were possible to print whole organs”, says Ms Laurent-Applegate, putting it into perspective. “Ultimately, it is up to the doctor to decide, in each individual case, whether it is in the patient’s interests to use 3D technology or whether traditional methods are best”. ⁄
The medical uses of 3D printing were pioneered in Switzerland. Phonak has been using it for ten years to produce shells for its hearing aids. “We make a 3D digital model of the ear canal, using a silicon impression, which is then sent for printing”, explains Stefan Launer, Vice Chairman of the company and head of science and technology. Such “large-scale made-to-measure production”, as he calls it, guarantees “better sound quality and greater comfort for patients”.
Zurich Children’s Hospital is currently developing another application of 3D technology, whereby fragments of skin are produced from the cells of burn victims, with a view to providing a graft. It uses the 3D printer developed by RegenHU, a Fribourg-based company which in February 2014 plans to launch “a bone substitute for transplanting into the jaw and increasing bone mass ahead of a dental implant”, describes boss Marc Thurner. It will be made of a synthetic material, but “with a biological microstructure that provides a sort of highway through which the patient’s cells can colonise”, he adds. Eventually these implants will be customised to suit the patient’s specific requirements. “If the recipient has diabetes or osteoporosis,for example, the implants can be impregnated with drugs to treat these conditions”, says Mr Thurner.
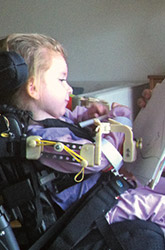
An exoskeleton made with a 3D printer allows 3-year old Stella to move her arms. Stella, who lives in Canada with her father, suffers from a genetic condition that affects her muscles.