
Medical laboratories now take much more than blood samples. Examining other parts of the body can improve the accuracy of diagnostics.
As every patient knows, the most common reason for visiting a medical laboratory is to have a blood or urine sample taken. These substances contain more than a thousand markers, such as toxins, proteins and hormones.
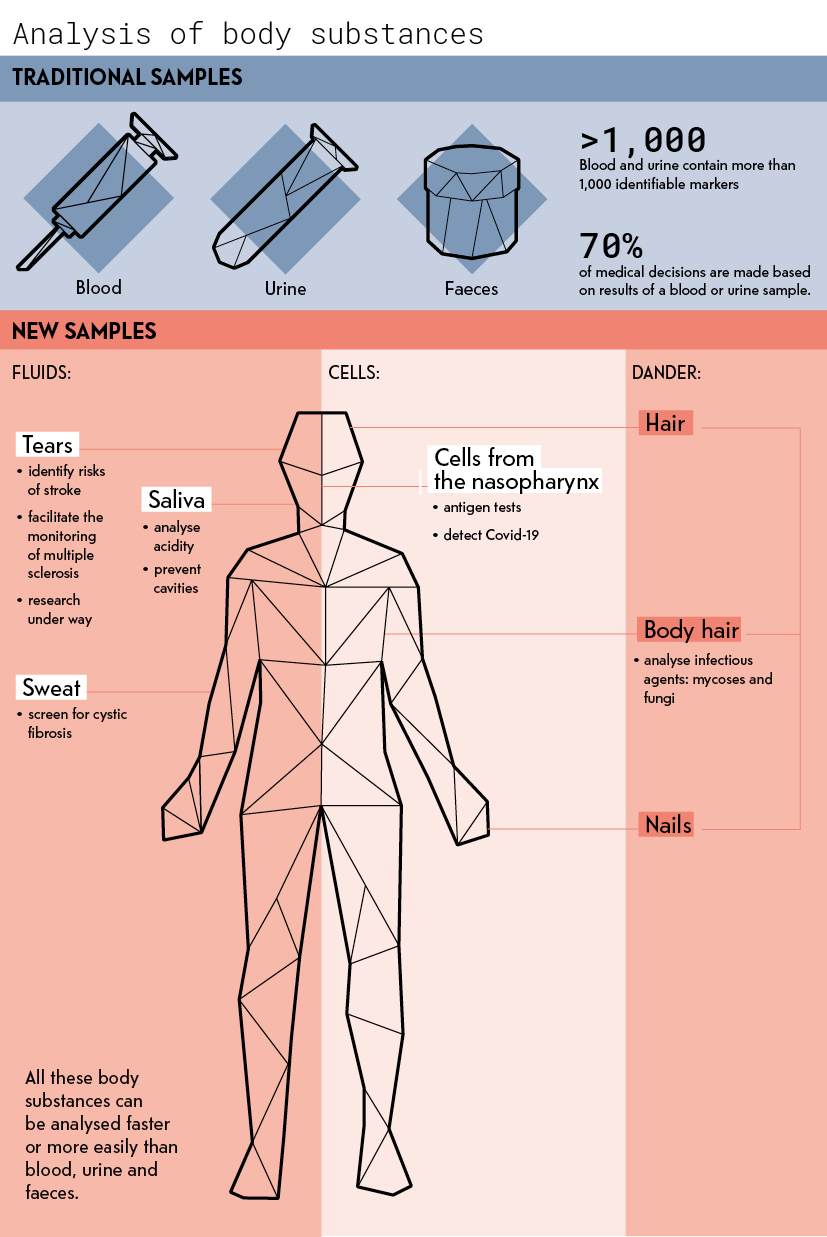
These in vitro tests are some of the most useful tools for health professionals. This type of exam is required in 70% of medical decisions. But practitioners and biologists now increasingly use other substances from the body. Sweat, tears and saliva tell us a lot about the state of our health, as do our hair, nails and body hair, or dander, to use the medical term.
There are several reasons for this new interest. Firstly, blood and urine testing has its limitations. Urine is rich in salts and crystals, which makes it difficult to detect certain protein biomarkers. In blood, albumin can mask other important indicators. Another problem is that “both of these substances tend to turn over too quickly in the system to detect certain chemical compounds that may have been present in the body over a long period,” says Olivier Gaide, physician in chief at the Service of Dermatology and Venereology at the CHUV. These elements can be found in other parts of the body much longer. For example, it takes six months to a year for a nail to completely regrow.
In everyday life, analysing our dander (nails and hair) or body fluids has another advantage. Taking the sample required is usually faster, easier and less painful than a phlebotomy – the fancy word for a blood sample. But that’s not always true. Anyone who has experienced a notorious nasal swab to test for Covid-19 knows that having biological samples taken is not always pleasant. The only solution available for several months, this technique involves inserting a swab up to the nasopharynx and rotating it to collect enough cells for a PCR or antigen test.
However, in most cases, alternatives to traditional blood samples are less painful, faster and easier, Olivier Gaide says. “A blood test is an invasive procedure, though only slightly, but some patients are put off by it. They prefer to provide biological samples without pain. Collecting saliva, tear fluid, hair, or nails is much easier.” These alternative tests also offer potential savings for healthcare systems. “Blood tests are costly and time-consuming. You need to have a quiet, isolated room, use disinfectant and phlebotomy equipment, mobilise staff, etc. But putting saliva in a tube or cutting a few hairs does not require any special skills.”
Stool analysis can be used to detect diseases, but also to restore a patient’s bacterial flora to treat various pathologies. Opened in 2019, the CHUV centre for faecal transplantation uses this technique for patients suffering from infection caused by a bacillus, Clostridium difficile, which causes severe diarrhoea and colitis. Mainly delivered in the form of capsules, the treatment has spectacular results. “Faecal microbiota transplantation (FMT) successfully treats 80% to 90% of patients, while traditional antibiotics are effective in 20% to 30% of cases,” says Tatiana Galperine, Chief Resident, who created the centre for faecal microbiota transplantation at the CHUV. The drug is currently undergoing a simplified market approval process with Swissmedic. But it is already used to treat some 30 CHUV patients a year.
“Our work also consists of selecting donors subjected to a particularly rigorous process,” Tatiana Galperine says. “Then there’s the production of the drug itself, in collaboration with the Infectious Diseases Services.” Finally, other activities are related to research, in particular working with the Service of Oncology. “Several studies suggest that FMT improves patient tolerance to certain chemotherapies or immunotherapies used to treat the digestive system.
It also appears to improve the response to these treatments by modulating the gut microbiota.” FMT has not said its last word.
The easy collection procedure lifts many constraints, especially advances continue to be made in medical devices, Olivier Gaide adds, citing the case of patients with diabetes. “The new blood sugar monitors prevent repetitive and painful blood tests. Patients can test their blood sugar every 15 to 30 minutes using a simple micro-needle patch, and adapt their insulin intake accordingly.”
Nails and hair are where Olivier Gaide focuses his attention. “Dander is useful for identifying infectious agents that attack a patient’s nail or hair system.” We combine several techniques, from the simplest to the most complex, to identify mycoses, moulds and yeasts. “The first examination is quick and painless. We take hair samples to look for fungi, either by removing part of the shaft or by pulling hairs out at the root to examine the bulb. We also regularly analyse nail fragments by inspecting them under a microscope and applying staining solutions if necessary to show the presence of a particular parasite.”
When necessary, a third phase of analysis involves placing the fragment in culture for a few days before performing a molecular biological examination that can detect the DNA of a pathogenic element.
Studying biological fluids or body materials is not a new practice. As far back as ancient times, doctors would examine the stool or urine of their patients. In the Middle Ages, a “salty kiss” referred to the taste of the skin of certain infants. Although the origin is unknown, this perspiration condition, which may indicate cystic fibrosis, is still routinely performed at the CHUV today. “We collect a small amount of sweat in a device placed on the child’s forearm after stimulating perspiration. Salt and chlorine levels are measured to confirm or most of the time rule out the diagnosis.”
Saliva tests are another valuable tool used by healthcare professionals. Dentists analyse saliva acidity and composition to prevent cavities and dental plaque. Saliva is easy to collect, does not expose healthcare professionals to transmissible blood-borne diseases, does not clot and contains over 1000 proteins and RNA molecules.
Like sweat, tears are one of the most promising fluids in terms of research. Ongoing clinical studies suggest that, within a few years, protein biomarkers or parasites in tear fluid will be used to detect a viral infection, identify risks of stroke and facilitate the monitoring of diseases such as multiple sclerosis, without the need to perform more cumbersome procedures such as lumbar punctures.
Analyses of the skin, nails and body fluids are valuable for patients and offer the prospect of being able to detect a wide range of biomarkers earlier and more accurately, as of the early stages of various diseases. This should open up new possibilities for doctors in the way they care for patients. /
“Alternatives to blood samples present advantages because they are less painful, faster and easier to perform.”